Participating states must have the approval of their legislatures. States could individually choose to license providers wishing to practice in their states or participate in a licensure compact with other states, providing reciprocity to the participating states. The provider must be licensed in the patient's state. 
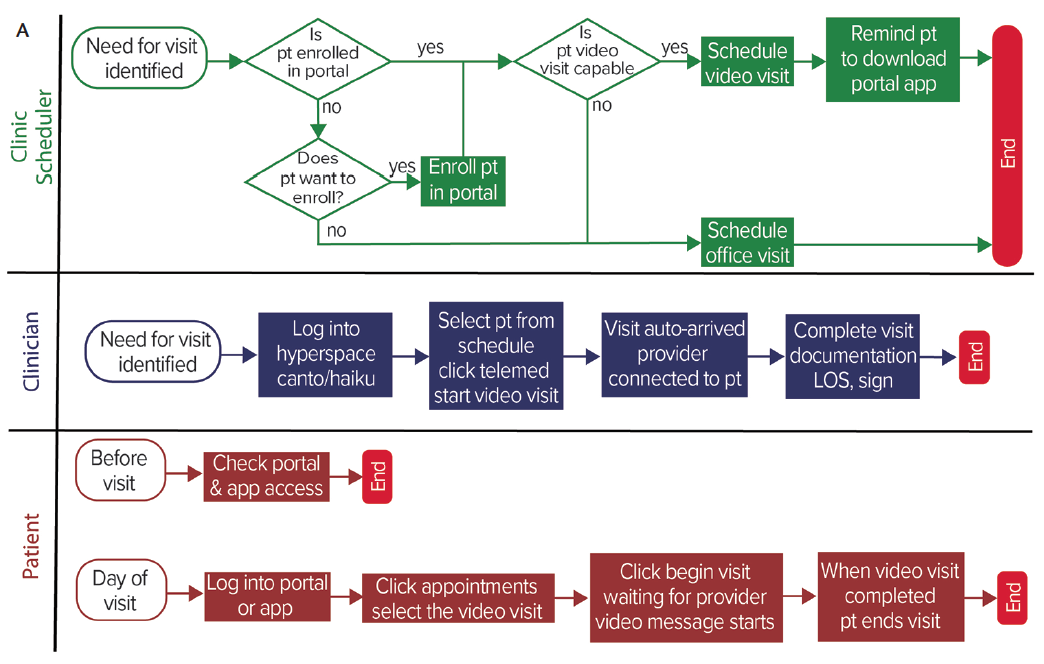
Licensing requirementīefore the PHE: Licensure of providers was and still is the purview of the individual states. Assignment means the healthcare provider has agreed to accept Medicare coverage as full payment.ĭuring the PHE: Providers providing telehealth services do not need to update their Medicare enrollment to include their home location, nor must their clinic/group practices do so if the provider has assigned his/her benefits. Their clinic/group practices were required to provide updated information if the provider had assigned his/her benefits. How the action occurred: CARES Act/1135 waiver Providers at homeīefore the PHE: Providers providing services from their homes were required to update their Medicare enrollment to include their home location. CMS encourages states to relax their licensing laws. The type of originating site had to be approved by CMS.ĭuring the PHE: Providers may deliver telehealth services to patients in their homes and other locations and in any area of the country. Provider/patient location Geographic and originating site requirementsīefore the PHE: Providers were reimbursed for services delivered to patients in an originating site located in a CMS-defined rural area. Unless an action taken during the PHE is made permanent either by statute or regulation, the action will expire when the PHE expires. Each category describes the statute or regulation before the PHE, the action taken during the PHE and how it occurred, the action that is being taken or could be taken following the expiration of the PHE. 
Medicare regulations: Medicare regulations for telehealth fall into seven categories. For example, under section 1135 of the Social Security Act, he/she may temporarily waive or modify certain Medicare, Medicaid, and Children's Health Insurance Program (CHIP) requirements to ensure that sufficient health care items and services are available to meet the needs of individuals enrolled in Social Security Act programs in the emergency area and time periods, and that providers who provide such services in good faith can be reimbursed and exempted from sanctions (absent any determination of fraud or abuse). Congress directed CMS to develop regulation/guidance and necessary waivers for these flexibilities.ġ135 Waiver: When the president declares a disaster or emergency under the Stafford Act or National Emergencies Act, and the Department of Health and Human Services (HHS) secretary declares a public health emergency under Section 319 of the Public Health Service Act, the secretary is authorized to take certain actions in addition to his/her regular authorities. It signaled strong support for the use of telehealth and virtual care and created flexibilities for previously created telehealth laws. The CARES Act: On March 27, 2020, Congress passed the Coronavirus Aid, Relief, and Economic Security (CARES) Act ( H.R.748), in response to the COVID-19 public health emergency (PHE). The Department of Health cannot provide legal guidance. It is for informational purposes only.Īlways consult with legal counsel when addressing legal and regulatory considerations. Disclosure: This information should not be regarded as legal advice. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
